Multifaceted Challenges: Increasing Vaccine Coverage in Burundi
In May 2022, Sabin’s Boost Community and the World Health Organization (WHO) launched the first cohort of the "COVID-19 Recovery for Routine Immunization Programs Fellowship". The aim of this program was to strengthen the capacity of national and sub-national immunization professionals to plan and implement immunization programming during the COVID-19 recovery period, with the ultimate goal of reversing the declining rates of immunization coverage. After an intensive live engagement series, Fellows were tasked with drafting their own strategic proposal for implementation or case study for publication. This series of Bright Spots share Fellows' key learnings and takeaways from the program.
Multifaceted Challenges: Increasing Vaccine Coverage in Burundi
Damien Bigirimana was working at a district hospital in Burundi when he first encountered children suffering due to missing out on essential vaccinations. He said, “When we did consultations, we found children with signs of vaccine-preventable diseases such as measles and newborn tetanus, and that worried me a lot.” He suspected the structure of health services contributed to this problem because vaccinations were not done at the hospital level. After being promoted to health center manager, immunization became a top concern of his work.
When Damien heard about the 2022 COVID-19 Recovery for Routine Immunization Programs Fellowship through a colleague, he jumped at the chance to apply. The Fellowship, offered by the Sabin Vaccine Institute’s Boost Community and the World Health Organization (WHO), provided an opportunity to strengthen the capacity of immunization professionals, like Damien, to recover and bolster immunization programs in their countries.
Identifying Vaccination Gaps
Damien’s vision was clear: he wanted to reduce the number of zero-dose children and improve vaccine coverage in Burundi by increasing confidence towards the COVID-19 vaccine. First, he identified a major gap in coverage in two health districts, Muramvya and Kiganda, in Muramvya Province: only 27 of 46 health centers had vaccination services, which undoubtedly contributed to low vaccine coverage in these areas. He hypothesized that vaccine confidence could be increased by building public trust in health services, fostering community engagement in childhood vaccination, and developing effective risk communication.
Damien’s team formalized a strategic plan of activities to be conducted in the Muramvya and Kiganda Health Districts, which was aided by learnings from the live sessions of the Fellowship. First, they held a coordination meeting of local partners working in the field of vaccination with community and religious leaders and the media. Next, they trained immunization providers on safety, managing and inputting immunization data correctly, and improving risk communication strategies. They also worked to strengthen vaccine safety to quell parents’ worries about giving their children the new COVID-19 vaccine. Then, they focused on reaching marginalized Batwa communities to mobilize awareness on the benefits of vaccination. Finally, the team analyzed vaccination data, alongside vaccinators, community representatives, and local associations involved in vaccination.

Practicing Perseverance to Uncover Zero-Dose Children
Bringing this plan to fruition was no easy feat. Damien describes the challenges faced on the ground as “multifaceted.” Several areas were inaccessible, which was compounded by the rainy season in the region. Rising fuel costs affected the available budget, and this limited some of the activities the team was able to carry out. Fighting poor perception of vaccination by certain segments of the community was especially difficult.
Additionally, Damien said, “the health centers revealed quality challenges in the vaccination service: vaccine management, lack of data analysis, lack of health education, and ineffective communication with mothers who bring children for vaccination.” Damien found that vaccination sessions, including health education, were often not offered to mothers prior to childhood vaccinations because providers assumed that mothers understood the process of vaccination completely. This contributed to parents’ mistrust in immunization, especially due to their fear of immunization side effects that they weren’t expecting, such as swelling at the injection sites and tears after injection. He emphasized the importance of health education to not only increase uptake of childhood vaccination but also to combat rumors surrounding the service. However, from the beginning of project implementation Damien noted positive changes. He said, “When I carried out a preliminary evaluation in one of the pilot health centers, I noticed that things had changed for the better in terms of the organization of the immunization service and the behavior of the providers.”
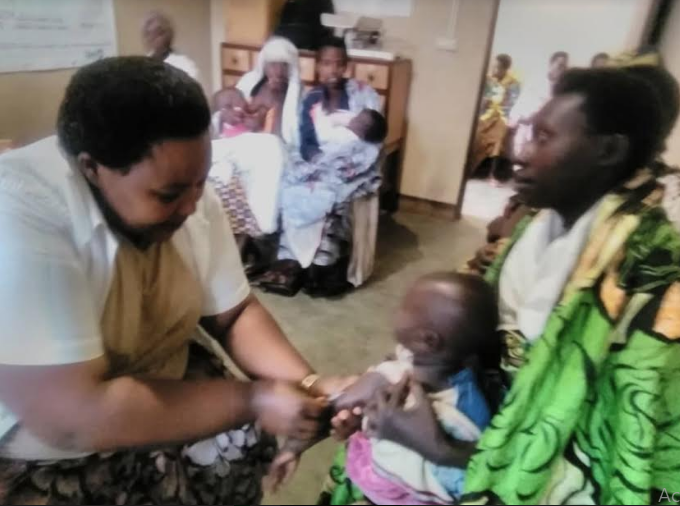
Ultimately, the team uncovered the most zero-dose children in Batwa communities, where they conducted mass vaccination campaigns in two villages and found that vaccination was not a community priority. Twenty undervaccinated and 34 zero-dose children were identified during implementation of the project –18 in Muramvya Health District and 16 in Kiganda Health District – all of whom were vaccinated. Furthermore, in Busangana Health Center in Muramvya Health District, several children with signs of measles were identified; their examinations were sent to a national laboratory which confirmed them as positive for measles. Muramvya Province was then identified as having a measles epidemic and, as a result, a nationwide measles vaccination campaign was organized.
Additionally, 112 health providers from the two districts improved their skills in the areas of security, management of vaccination inputs, and Expanded Programme on Immunization (EPI) communication and 14 Health Promotion Technicians and 20 community representatives were trained in EPI communication. As a result of this training, health providers noted that there was improved risk communication and changes in the speed and accuracy of data inputs on vaccinated children.
Final Results
20 under-vaccinated children were identified and vaccinated
14 zero-dose children were identified and vaccinated
112 health providers improved their skills in the areas of security, management of vaccination inputs, and EPI communication
14 Health Promotion Technicians were trained in EPI communication
20 community representatives were trained in EPI communication
The mobilization awareness campaign conducted in two Batwa communities was successful in encouraging community members to get vaccinated, and Damien emphasized that the perception of the importance of immunization has noticeably improved in these communities. Damien advises that specific communication must be carefully crafted to mobilize certain populations that are vaccine hesitant, especially those that are marginalized.
Damien’s vow to improve immunization coverage in his country is unwavering. He said, “I am committed to promoting child and family health in my country and throughout the world, whatever the situation.” Implementation of his project is ongoing, and he hopes to make further strides in increasing vaccine confidence and coverage in Burundi.

2022 Fellow & Contributor
Damien attended Mwaro Community University and obtained a Bachelor's degree in Sciences and Paramedical Techniques. Since 2015 he has served as health supervisor for the province of Muramvya, with responsibility for vaccination, pharmacovigilance and reproductive health.